When Your Toenails Start Changing
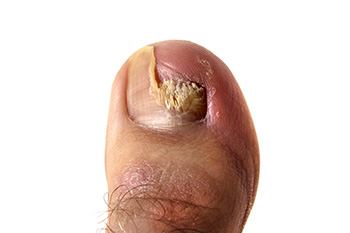
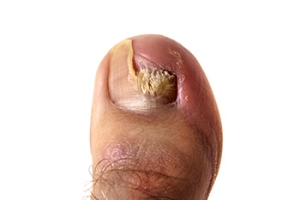
Toenail fungus does not appear overnight, but once it takes hold, it is hard to ignore. At first, a small white or yellow spot may appear on the toenail. Over time, the nail thickens, turns yellow or brown, and may become brittle, crumbly, or even lift from the nail bed. Some people experience a foul odor, while others feel discomfort when wearing shoes. Treatment takes patience. Mild cases may improve with antifungal creams or medicated nail lacquers, but more stubborn infections often require prescription oral medication or laser treatments. In severe cases, the nail may need to be removed. Prevention is key. Keep feet clean and dry, wear breathable shoes, and avoid walking barefoot in public places like around pools or in locker rooms. Trim nails straight across and disinfect nail clippers. If the infection persists, it is suggested that you see a podiatrist who can recommend the best course of action.
For more information about treatment, contact Dr. Michael A. Wood of Foot Health Institute. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Toenail Fungus
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment that fungal infections thrive in. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids and creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
Painful Plantar Fasciitis

Plantar fasciitis is perhaps the most common cause of heel pain. It results from inflammation of the thick band of tissue called the plantar fascia, that runs along the bottom of the foot. The primary symptom is sharp, stabbing pain in the heel, particularly when taking your first steps in the morning or after sitting for a while. The pain can lessen with movement but may return after long periods of standing or walking. This condition is often caused by repetitive strain on the plantar fascia, which can be triggered by activities like running, wearing improper footwear, or having flat feet or high arches. A podiatrist can diagnose plantar fasciitis through a physical exam and may use imaging tests for a clearer view. Treatment typically involves stretching exercises, custom orthotics, and anti-inflammatory medication. In more severe cases, corticosteroid injections may be recommended. If you are dealing with this condition, it is suggested that you schedule an appointment with a podiatrist for proper care and relief.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
How to Manage the Onset of Flat Feet
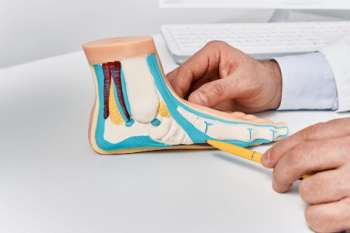
Progressive collapsing foot deformity, also known as adult-acquired flatfoot, occurs when the arch gradually collapses, leading to changes in your foot’s shape and function. Adult-acquired flatfoot often results from dysfunction in the posterior tibial tendon, which plays a key role in supporting the arch and turning the foot inward. As this tendon weakens, the foot may flatten, and the alignment of the ankle can shift, sometimes causing pain or difficulty walking. Aging, previous injuries, obesity, diabetes, or arthritis may contribute to the development of adult-acquired flatfoot. It may result in pain along the inside of the ankle, swelling, or an outward shift of the foot’s position. A podiatrist can assess the severity of the condition using certain imaging tests to determine the best course of treatment. Supportive devices, orthotic inserts, and in more advanced cases, surgery, may help restore function and relieve pain. If you notice that your feet have become flatter, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flat Feet
Flatfoot is a condition that occurs when the arches on the foot are flattened, which allows the soles of the feet to touch the floor. Flatfoot is a common condition and it is usually painless.
Throughout childhood, most people begin to develop arches in their feet, however, some do not. Those who do not develop arches are left with flatfoot. The pain associated with flat feet is usually at its worse when engaging in activity. Another symptom that may occur with those who have this condition is swelling along the inside of the ankle.
It is also possible to have flexible flatfoot. Flexible flatfoot occurs when the arch is visible while sitting or standing on the tiptoes, but it disappears when standing. People who have flexible flatfoot are often children and most outgrow it without any problems.
There are some risk factors that may make you more likely to develop flatfoot. Those who have diabetes and rheumatoid arthritis have an increased risk of flatfoot development. Other factors include aging and obesity.
Diagnosis for flat feet is usually done by a series of tests by your podiatrist. Your podiatrist will typically try an x-ray, CT scan, ultrasound, or MRI on the feet. Treatment is usually not necessary for flat foot unless it causes pain. However, therapy is often used for those who experience pain in their flat feet. Some other suggested treatment options are arch supports, stretching exercises, and supportive shoes.
Arthritis Can Cause Pain in the Feet and Ankles
Explanation of Hammertoe
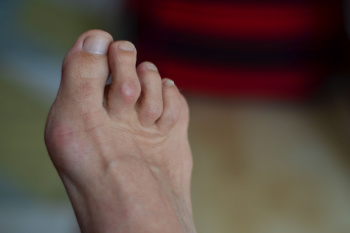
Hammertoe occurs when one or more of the smaller toes become bent in a Z-shaped position, due to an imbalance in the tendons or poor joint alignment. Common causes of hammertoe include wearing ill-fitting shoes, having unusually long toes or metatarsal bones, or conditions like rheumatoid arthritis. The second toe is most frequently affected, but the third and fourth toes can also develop into a hammertoe. This deformity often results in discomfort when wearing shoes, especially those with a narrow or low-toe box. Excessive friction on top of the affected toe can lead to calluses, corns, or even ulcers. In some cases of hammertoe, pain in the ball of the foot, known as metatarsalgia, develops. A podiatrist can diagnose hammertoe through an examination of the foot while assessing other joints for arthritis or other underlying conditions. Treatment options include custom orthotics to reduce pain or surgical correction for rigid deformities. If you have developed a hammertoe that is causing discomfort, it is suggested that you make an appointment with a podiatrist for an exam and treatment options.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
- Pain in the affected toes
- Development of corns or calluses due to friction
- Inflammation
- Redness
- Contracture of the toes
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions please contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Hammertoe
Hammertoe is a foot deformity that occurs due to an imbalance in the tendons, muscles, or ligaments that are responsible for holding the toes in their normal position. This condition may be caused by poor footwear, foot structure, trauma, and disease. The most common solution for hammertoe is to relieve the pain by changing your footwear and wearing orthotics. In severe cases, surgery may be required.
The shoes that are most likely to cause hammertoe are high heeled shoes or shoes that are too tight in the toe box. Tight shoes will force your toes to crowd together in a curled position. This position will likely continue when you take your shoes off. Another cause is trauma. When you stub your toe, you are increasing the chance that you will develop hammertoe.
There are risk factors that may make you more likely to develop this condition. Women are more likely to have the condition compared to men, and it is also more likely to appear in those who are older in age.
Many different foot problems can be avoided by wearing shoes that have adjustability, adequate toe room, and low heels. Furthermore, if you want to buy new shoes, you should look to purchase them at the end of the day and make sure you know your correct size. The importance of buying shoes at the end of the day is that your feet swell as the day progresses. You should also ensure that you are wearing your correct size because your shoe size may change as you grow older.
To diagnose someone with hammertoe, your podiatrist will need to conduct a thorough examination of your foot. Your doctor may even order an x-ray to evaluate the bones and joints of your feet and toes.
If you have hammertoe, your podiatrist may recommend that you wear shoes that fit you better along with inserts to place inside them. Additionally, he or she may suggest special exercises for you to perform to stretch your toes. One helpful exercise it to pick up marbles with your feet or crumple a towel with your toes.
Prior to meeting with your podiatrist, it will be helpful to make a list of all the symptoms you are experiencing. You should also make a note of medications you are taking and important personal information about your medical history.
Pickleball and Ankle Fractures

Ankle fractures are a growing concern in pickleball, particularly among older women. Post-menopausal players are at greater risk due to reduced bone density, making bones more susceptible to breaks. These injuries often occur during falls when a player slides or dives for the ball but miscalculates their landing, leading to a painful twist or impact. An ankle fracture involves a break in one or more of the bones in the ankle joint, causing swelling, bruising, and difficulty bearing weight. Preventing such injuries starts with wearing sturdy, supportive shoes designed for court sports and improving balance and agility through regular exercise. Playing on well-maintained surfaces and practicing controlled movements also help reduce risks. If you have broken your ankle while playing pickleball, it is suggested that you visit a podiatrist for appropriate treatment.
Broken ankles need immediate treatment. If you are seeking treatment, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.