
Toe pain can signal an underlying issue with how blood flows to and from the lower extremities. Because the toes are farthest from the heart, they are often affected first when circulation becomes compromised. Signs of poor circulation include coldness, color changes such as pale, bluish, or reddish tones, or swelling that worsens throughout the day. Some people notice numbness, tingling, or even pain during walking that subsides with rest, which can indicate restricted blood flow. Discoloration or thickened toenails, especially when accompanied by slow healing of minor cuts or sores, may also suggest poor circulation. People with diabetes are especially vulnerable, as nerve damage and vascular disease can reduce blood supply and increase the risk of infections or tissue damage. A podiatrist can conduct a thorough examination and order diagnostic testing to determine the cause. Treatment may involve medication, circulation assessments, or surgery, in more severe cases. If you are experiencing toe pain, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Dr. Michael A. Wood of Foot Health Institute. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
- Muscle pain, stiffness, or weakness
- Numbness or cramping in the legs
- Skin discoloration
- Slower nail & hair growth
- Erectile dysfunction
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
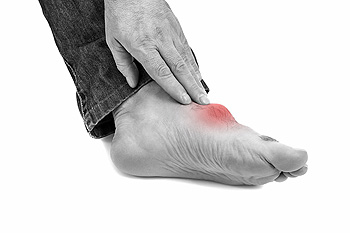
Gout is a form of inflammatory arthritis that develops when uric acid builds up in the blood and forms sharp crystals in the joints. The big toe is one of the most common locations for a gout attack due to its lower temperature and reduced circulation compared to other areas. Early signs of gout often begin suddenly and may include intense pain, swelling, redness, and warmth in the affected toe. The joint may become extremely tender, making it difficult to walk or wear shoes. These symptoms often appear during the night and can worsen quickly. Gout can be extremely painful, and may cause difficulty in completing daily activities. If you have symptoms of this condition, it is strongly suggested that you are under the care of a podiatrist who can offer you relief, management and prevention tips.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Some athletes continue to feel ankle pain long after a sprain has healed. This ongoing discomfort can be caused by hidden damage inside the joint, like scar tissue or small tears. When rest, targeted exercises, and other treatments do not bring relief, a procedure called arthroscopic surgery may be helpful. It uses tiny tools and a camera to look inside the ankle and fix the problem without large cuts. This kind of surgery can reduce pain and help athletes get back to their sport more safely and comfortably. If you are still having ankle pain after a past injury, it is suggested that you visit a podiatrist to explore the best options for healing, which may include arthroscopic surgery.
Sports related foot and ankle injuries require proper treatment before players can go back to their regular routines. For more information, contact Dr. Michael A. Wood of Foot Health Institute. Our doctor can provide the care you need to keep you pain-free and on your feet.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are a common occurrence when it comes to athletes of any sport. While many athletes dismiss the initial aches and pains, the truth is that ignoring potential foot and ankle injuries can lead to serious problems. As athletes continue to place pressure and strain the area further, a mild injury can turn into something as serious as a rupture and may lead to a permanent disability. There are many factors that contribute to sports related foot and ankle injuries, which include failure to warm up properly, not providing support or wearing bad footwear. Common injuries and conditions athletes face, including:
- Plantar Fasciitis
- Plantar Fasciosis
- Achilles Tendinitis
- Achilles Tendon Rupture
- Ankle Sprains
Sports related injuries are commonly treated using the RICE method. This includes rest, applying ice to the injured area, compression and elevating the ankle. More serious sprains and injuries may require surgery, which could include arthroscopic and reconstructive surgery. Rehabilitation and therapy may also be required in order to get any recovering athlete to become fully functional again. Any unusual aches and pains an athlete sustains must be evaluated by a licensed, reputable medical professional.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

